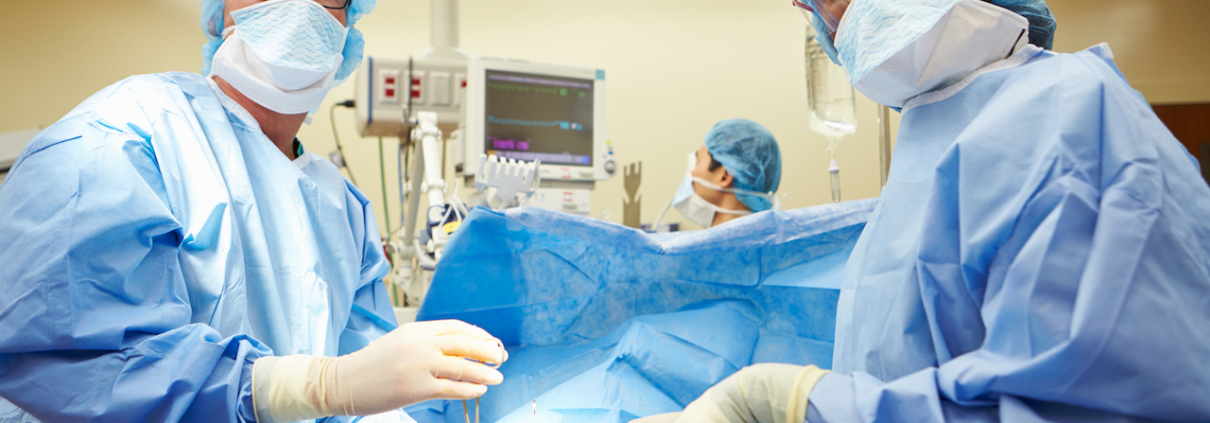
When & What Type of PPE Should Be Used: NHS & Healthcare
The NHS introduced new guidelines for personal protective equipment (PPE) in April 2020. They said:
“Any clinician working in a hospital, primary care or community care setting within two metres of a suspected or confirmed Covid-19 patient should wear an apron, gloves, surgical mask and eye protection.”
The guidelines also stipulated that clinicians should wear “a higher level of protective equipment” when carrying out aerosol generating procedures (AGPs).
These guidelines stipulated that healthcare workers essentially wore personal protective equipment round the clock. But this was during a global pandemic, when people from all walks of life took special measures to reduce the risk of infection.
So what are the PPE guidelines for NHS and healthcare workers during “normal times”, when we’re not fighting to contain a new virus?
A Brief Introduction to PPE
When we talk about PPE, we’re mainly referring to the following equipment:
- Head covers, for facial and head hair
- Masks and face shields
- Scrubs
- Gowns and aprons
- Gloves
- Footwear
All PPE fulfils the same essential function: to prevent the spread of viruses and bacteria, and to protect both staff and patients from contamination and infection.
Certain specialist procedures might call for specialist PPE precautions. For example, many healthcare settings have specific PPE guidelines for staff involved in chemotherapy treatments.
But by and large, when we refer to PPE, we’re referring to the above equipment.
When & What Type of PPE Should Be Used – Latest NHS Guidance
The NHS published the latest National Infection Prevention and Control (IPC) manual in June 2022. Though these guidelines apply to healthcare settings in England, the guidelines in Scotland, Wales and Northern Ireland will be broadly similar.
These guidelines reinforce the important role PPE plays as a standard infection control precaution (SICP).
Healthcare workers should assess the risks associated with any procedure before deciding what PPE to use:
“Before undertaking any procedure, staff should assess any likely exposure to blood and/or other bodily fluids, non-intact skin or mucous membranes and wear personal protective equipment (PPE) that protects adequately against the risks associated with the procedure.”
Basic PPE Principles in Healthcare
Regardless of the patient and the procedure, the latest NHS guidelines say that all PPE must be:
- Stored close to the point of use in a clean, dry area
- Single-use only, unless specified by the manufacturer
- If reusable, decontaminated after use according to the manufacturer’s instructions
- Changed immediately after seeing each patient, or after completing a procedure or task
- Disposed of immediately after use in the correct waste stream – domestic, non-infectious, or clinical
- Discarded immediately if it gets damaged or contaminated.
Read our full guide to the factors to consider when choosing PPE.
Beyond this, there are specific guidelines for each type of PPE.
NHS Glove Guidelines
The NHS advises that gloves must be worn when there’s any chance that a procedure will involve exposure to blood, other bodily fluids, non-intact skin or mucous membranes. Though it’s not recommended for routine clinical care, some exposure-prone procedures may require double gloving – such as gynaecological or orthopaedic operations, and major trauma incidents.
Do I Need to Wear Gloves When Using the Phone or Computer in a Hospital?
Gloves are not necessary for administration tasks, even if you perform them near patients – such as using telephones or computers, distributing or collecting food, writing in the patient chart or giving oral medication.
When to Change Gloves in Healthcare?
You must change your gloves immediately after seeing each patient, and after performing any task or procedure – even if it’s with the same patient. You must also change your gloves immediately if you suspect they have a perforation or a puncture.
NHS & Healthcare Apron and Gown Guidelines
Wear aprons to protect your uniform or clothes when you anticipate contamination – such as when in direct care contact with a patient. And like gloves, you must change your apron after seeing each patient, or after completing each task or procedure.
When to Wear Gowns instead of an Apron?
Wear gowns or coveralls instead of aprons when there’s a risk of extensive splashing of blood or bodily fluids, such as in the operating theatre or the intensive care unit. Gowns too must be changed between patients and procedures. And any gowns or coveralls worn in an operating theatre must be sterile.
NHS Face Protection Guidelines
You must wear eye or face protection, such as a full-face visor, whenever you anticipate any blood or bodily fluid contamination to the eyes or face. This includes during surgical procedures, and “always during aerosol generating procedures.”
The guidelines stipulate that regular corrective spectacles do not count as eye protection, and that any protection you wear should not be impeded by piercings, false eyelashes or other accessories.
NHS Mask Guidelines
When it comes to masks, the guidelines only cover fluid-resistant surgical face masks (FRSM). They recommend using these as a means of source control – to protect the patient during sterile procedures, such as surgery. They also recommend using them whenever there’s a risk of splashing or spraying of blood or other bodily fluids.
Like all PPE, the guidelines stipulate that you should remove or change your mask regularly – at the end of each task or procedure, and if the mask’s integrity gets breached (by moisture build-up, for example).
The guidelines also make it clear that face protection is only effective it it’s well-fitting. A specialist face-fit testing service will help you ensure that all of your PPE is fit for purpose.
NHS Footwear Guidelines
While the guidelines don’t specify what specific type of footwear to use for general clinical work, they do stipulate that all footwear must be “visibly clean, non-slip, and well-maintained.” What’s more, any shoes you wear must be supportive, and they must cover the whole foot to avoid contamination and injury.
In areas where dedicated footwear is required, such as the operating theatre, you must remove the footwear before leaving the designated care area.
NHS Headwear Guidance
Unlike most PPE, headwear is not routinely required in clinical areas. It’s only required when it’s necessary to prevent contaminating the environment, such as in operating theatres, central decontamination units, and clean rooms.
But like all PPE, any headwear must be changed or disposed of between clinical procedures or tasks. And it must be removed before leaving the sterile environment. The headwear must completely cover the hair, and if you have any facial hair, you must cover this too, with a snood.
There are separate guidelines for headwear worn for religious regions, including turbans and headscarves. While staff do not have to remove this headwear, they must ensure they do not compromise patient care and safety. So any headwear must be washed or changed daily, and removed immediately if it gets contaminated. And staff must still comply with additional attire in operating theatres and other controlled environments.
Other Standard Infection Prevention Procedures
PPE is vital, but it’s just one part of the infection prevention jigsaw. Other important factors include hand hygiene, cough and respiratory hygiene, waste disposal, and fluid management.
You can read the latest NHS national IPC manual for England.
You can also read our guide to cleaning for infection control in operating theatres.
If you need extra advice and support, we specialise in infection prevention and control.
Our services include:
- Air purification consultations and solutions
- Face-fit testing
- Fluid management and washroom hygiene solutions
- Comprehensive infection control solutions, such as cleaning equipment and sanitising chemicals