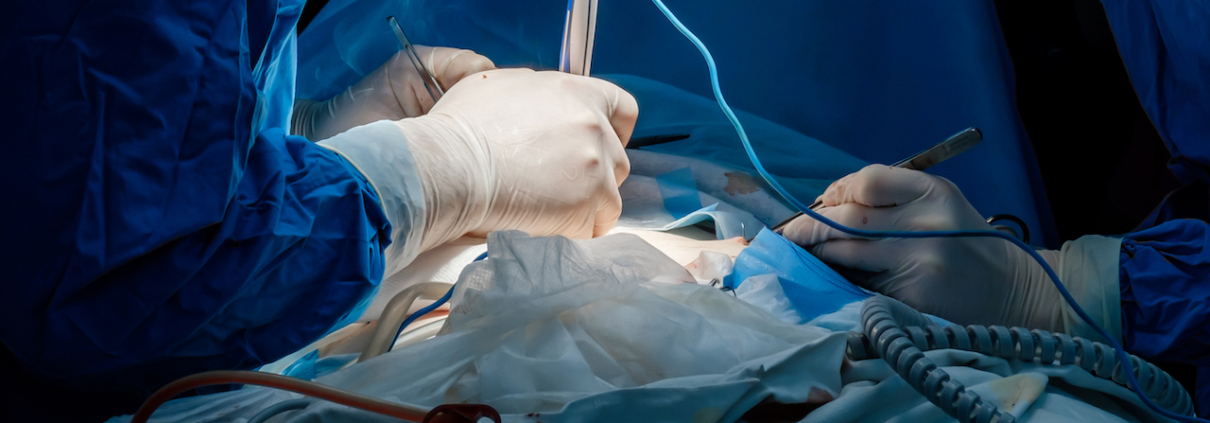
What’s The Difference Between Electrosurgery and Electrocautery?
Electrosurgery and electrocautery seem like broadly similar processes, as both involve making use of electrical currents in surgical procedures, and both involve cauterising wounds to limit blood loss.
But despite their similar names, the two processes are actually highly distinct, and each is used to achieve a specific outcome in a surgical setting.
So in this post we’ll explain the difference between electrosurgery and electrocautery by exploring each process, in turn.
What is Electrosurgery?
Electrosurgery involves using an electrical current to cut, remove or destroy tissue while controlling bleeding. Electrosurgical equipment operates at high frequencies. During procedures, electrical currents are passed through an electrode that’s placed on or near the tissue – with the electrical current entering the patient’s body.
Electrosurgery is used to remove abnormal cells in the treatment or prevention of certain cancers. It can also be used to treat other skin conditions, including warts and moles.
What is Electrocautery?
Electrocautery involves using a direct or alternating current to destroy abnormal tissue, such as a tumour or a legion, or to control bleeding in an injury after surgery. The electrical current is used to heat an electrode which is then placed on or near the tissue, with no electrical current passing into the patient’s body.
What’s The Difference Between Electrosurgery and Electrocautery?
In electrosurgery, the electrical current enters the patient’s body. But during electrocautery processes, the current never enters the patient’s body. Electrosurgical equipment is also invariably more elaborate than electrocautery units. Electrocautery equipment can involve small, battery-powered devices. While these are usually reusable, they can also be disposable.
The Risks of Electrosurgery and Electrocautery
In electrosurgery, the patient forms part of the electrical current, so surgical teams will have to take special precautions before the procedure to ensure both staff and patient safety. But in electrocautery, the current flows through an electrode, generating heat instead. The surgeon then uses the direct transfer of heat to burn tissue or cauterise wounds.
However, as both processes involve using electrical currents and heat as part of delicate surgical procedures, both electrosurgery and electrocautery procedures can generate surgical plumes – or surgical smoke.
Surgical smoke can produce an immediate hazard for surgeons through obstructing their view of the surgical site. But a more pressing concern is that surgical plums can contain numerous toxic gases, particulates, viruses, bacteria and other harmful vapours.
One study found that surgical smoke contains acrylonitrile and hydrogen cyanide. These are volatile, colourless, and toxic chemicals that can be absorbed into the lungs through the skin and via the gastrointestinal tract. So exposure to surgical smoke has been linked to eye, nose and throat infections, coughs and nasal congestion, and asthma and asthma-like symptoms, including breathing difficulties.
Managing the Risks of Surgical Plumes
We have a couple of guides on our site to help you understand and manage the risks of surgical smoke:
- Surgical Smoke Hazards: Causes and Exposure
- Effective Diathermy Smoke Plume Management in Operating Theatres
Our workplace exposure monitoring will help you meet your COSHH obligations anywhere your staff and patients are exposed to hazardous substances in your hospital – such as surgical plumes. Get in touch to talk to an air purification expert today.
We also specialise in air purification in healthcare settings. Our Blueair Health Protect 7440i Air Purifier can completely filter the air in a room of up to 38m² 4.8 times per hour. Its advanced filters can trap and kill up to 99.9% of potentially harmful particles in the air, including viruses, bacteria, and the hazardous chemicals contained in surgical smoke.