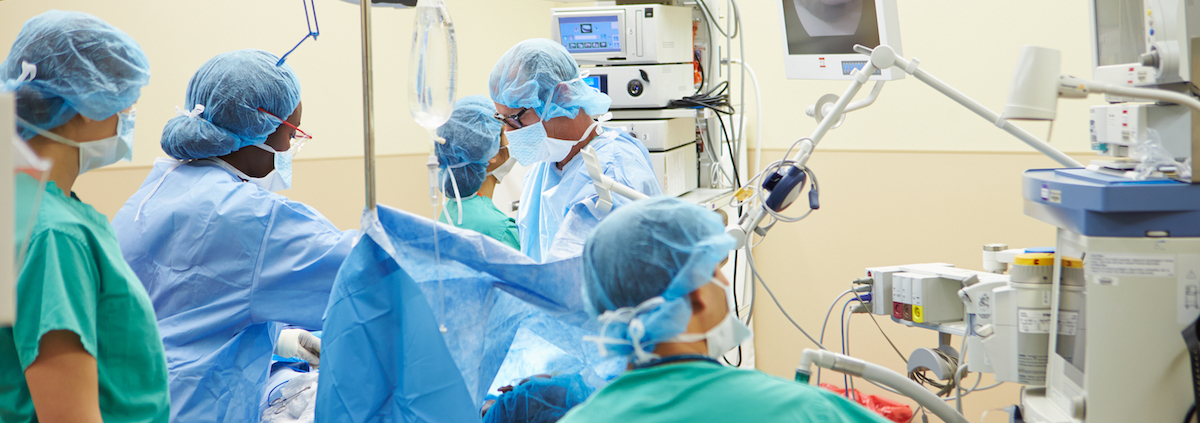
Operating Theatre Temperature & Humidity Guidelines For Patient Safety and Infection Control
Good air ventilation is an integral part of effective infection control in operating theatres. But while it’s important to keep the air circulated, it’s equally important to ensure the air is at the optimum temperature and humidity.
Why is Temperature and Humidity Important in an Operating Theatre?
For temperature and humidity levels to be right, there are three crucial needs:
- To avoid humidity levels that could cause risks with the anaesthetic.
- To ensure that operating theatre staff can work comfortably and efficiently.
- Perhaps most crucially, to ensure the patient’s not so cold that they risk developing hypothermia or cardiac arrhythmia, but not so hot that they experience heat stress.
Both staff and patients will potentially spend many hours in an operating theatre environment. And while in the theatre, the staff will be undertaking intensive, high-pressure work, while the patient will be in a profoundly vulnerable state. So the temperature and humidity in an operating theatre needs to be just right.
Operating Theatre Temperature and Humidity Guidelines UK
The Association for Perioperative Practice (AfPP) and The National Institute for Health and Care Excellence (NICE) have both issued guidelines for temperature and humidity control in operating theatres.
To best suit the needs of both staff and patient:
- The temperature should be maintained between 18 and 25°C, varied within this range depending on the patient and the procedure.
- The relative humidity should be 50%, to allow for tolerable working conditions for the long-term with no risk of anaesthetic issues.
NICE also outlines that theatre staff should measure a patient’s temperature every 30 minute during their operation, and that their temperature should be at least 21°C at any times when they’re not covered.
Other Safety Measures in Operating Theatres
Maintaining the correct temperature and humidity in the operating theatre is essential for both staff and patient safety.
But this is just one aspect of a safe and productive operating theatre. In addition to temperature control, the following measures are crucial:
Zoning for Infection Control
The theatre complex should be zoned based on cleanliness levels, the presence of microorganisms, and the types of procedures carried out. There must also be separate areas for all the key processes – preparation, disposal, scrubbing, gowning, and equipment storage, sterilisation, and washing.
Operating Theatre PPE
Staff should use the appropriate PPE for the procedure. They should apply their PPE in the correct order, and in a dedicated area, while thoroughly washing their hands at key points throughout the procedure. Also, any PPE they use should be properly fitted to ensure its effectiveness.
Equipment Cleaning
Any reusable surgical equipment should be thoroughly cleaned before use. And once processed, all surgical equipment must be correctly stored in a sterile environment, and not handled until it’s ready to be used on patients. Absorbent mats can also be used to capture fluids during procedures for quick disposal afterwards.
For more, you can read our complete guide to cleaning for infection control in operating theatres.
Support For Infection Control in Operating Theatres
It’s up to your hospital management and your theatre teams to maintain the optimum temperature and humidity settings in your theatre environments. But we can help you with many other aspects of infection prevention and control, helping you to meet all relevant standards while keeping your staff and patients as safe and as comfortable as possible.
Our services include:
- Air purification consultations and solutions.
- Face-fit testing.
- Fluid management and washroom hygiene solutions.
- Comprehensive infection control solutions, such as cleaning equipment and sanitising chemicals.